Varicose Veins
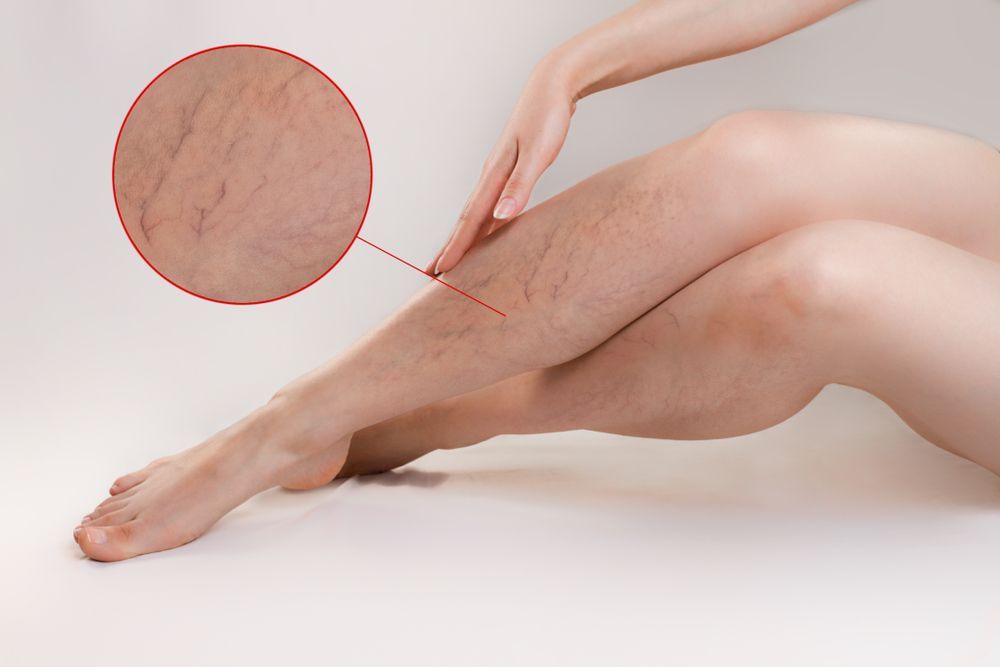
What are varicose veins?
Varicose veins are twisted, bulging veins that sit just below your skin’s surface (superficial veins). According to the University of Rochester Medical Center, nearly 40 million adults in the United States have varicose veins. If you have these veins in your legs or calves, you are not alone. Up to 70 percent of women and 40 percent of men will develop them by age 60.
For some people, varicose veins are part of the normal aging process — for others, they may be a sign of underlying vein issues. While they are not life-threatening, varicose veins can be uncomfortable and troublesome. If they are left untreated, they can eventually lead to other health complications. Learning the symptoms of these veins and what causes them can help you get the treatment you need from a vascular specialist.
How Do Veins Work?
To better understand how varicose veins form, it is important to first learn how your body’s veins work. Veins are blood vessels that are responsible for carrying oxygen-depleted blood from your tissues back toward your heart and lungs. There are three different types of veins — deep veins, superficial veins, and perforating veins.
Deep veins are the largest veins in your body, which are found inside your muscles. Around 90 percent of the blood in your legs is found in the deep veins. These veins also have one-way valves that help ensure blood moves away from your legs and toward your heart. Your calf muscle squeezes when you walk, which acts like a “second heart” to help pump blood from the deep veins in your leg.
Superficial veins are smaller veins found close to your skin’s surface. These veins move blood from the tissues near the skin back into your deep veins. The largest vein in your body is the great saphenous vein — this is a superficial vein that runs along your leg from your ankle to your thigh. It is important to note that blood moves more slowly through superficial veins compared to deep veins because they are not squeezed by the calf muscle.
The perforating veins act as short passageways between the superficial veins and deep veins. These veins also have valves that close when your calf muscle squeezes to prevent blood from the deep veins from flowing backward into the superficial veins (known as venous reflux).
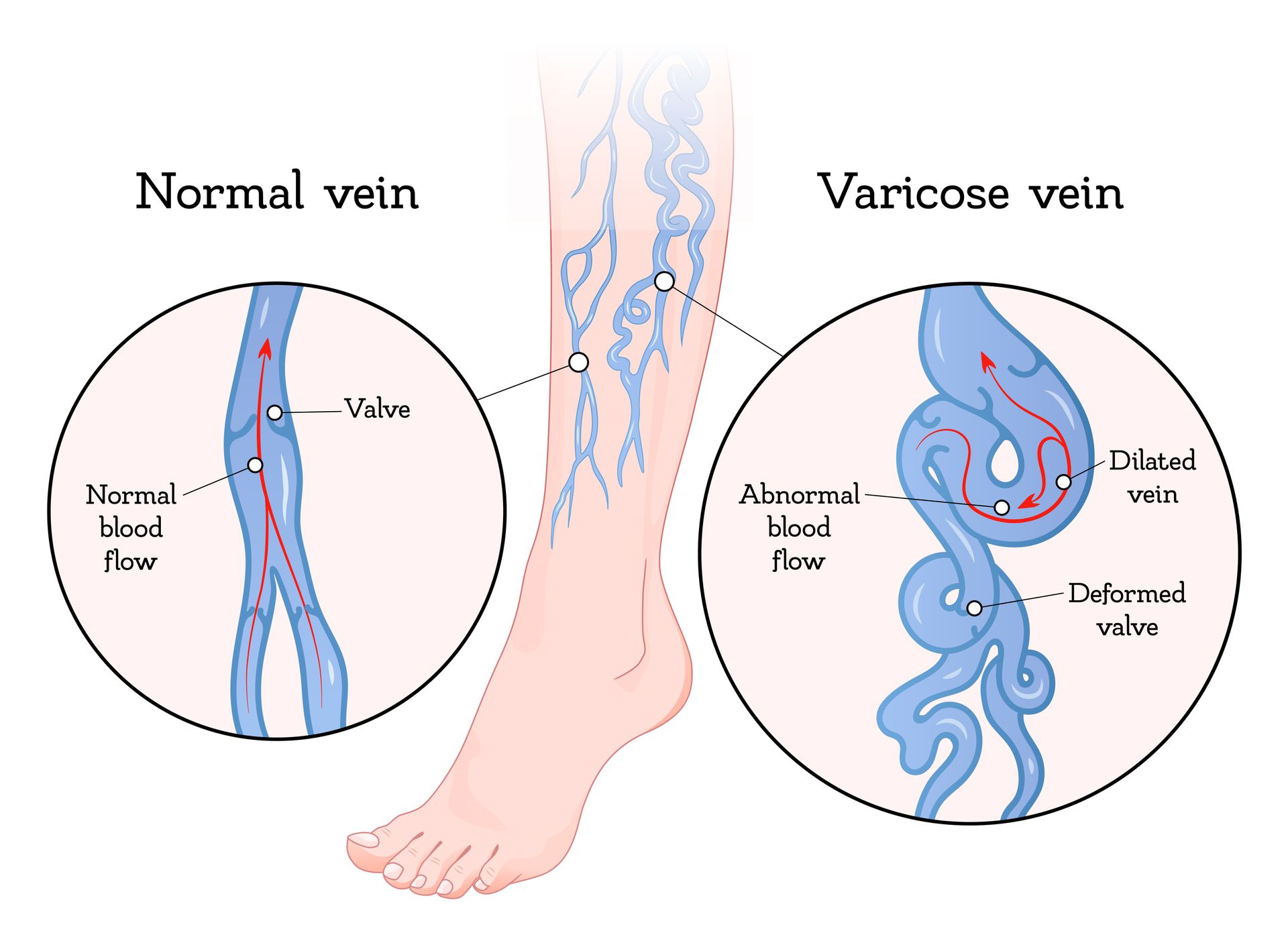
How Do Varicose Veins Form?
Most people with varicose veins also have a condition known as venous insufficiency. This is caused by increased pressure in your legs’ blood vessels. Over time, this pressure buildup widens (dilates) and weakens the vein walls. The valves also become damaged, causing blood to pool or flow backward into your leg toward your skin’s surface. When blood pools in your superficial veins, they begin to swell, change shape, or bulge outward. These are known as varicose veins.
While most varicose veins are harmless, they may be a sign of more severe venous disease. Chronic venous insufficiency (CVI) is diagnosed when you have both varicose veins and swelling (edema) in your legs. Varicose veins on their own are not considered CVI — however, they may be a sign of future damage. If you notice any new varicose veins or swelling, talk to your doctor or book an appointment with a vein specialist. They can help you address any problem veins before they become worse.
To learn more about CVI,
read here.
Risk Factors and Causes of Varicose Veins
Certain risk factors increase your chances of developing varicose veins. Some of these you can control, while others you cannot. Your doctor or a vein specialist can help you better understand what your risks are and the steps you can take to prevent new or worsening varicose veins.
Family History and Genetics
If you have a family history of varicose veins or venous insufficiency, you are more likely to develop these conditions yourself. Doctors and researchers have found that certain genes involved in how the skeletal and vascular systems develop can increase your risk of varicose veins. These genes are passed down through families from parents to their children.
Varicose veins are also caused by congenital disorders that are diagnosed at birth. Many of these disorders are also passed down through family members. They include:
- Ehlers-Danlos syndrome: a condition that affects the connective tissues (blood vessel walls, skin, and joints)
- Severe congenital neutropenia: a condition caused by low levels of certain immune cells known as neutrophils
- Klippel-Trenaunay syndrome: a condition that affects the development of blood vessels, bones, skin, and muscles
Pregnancy
Women — in general — are more likely to develop varicose veins than men. Hormonal changes from pregnancy also contribute to this increased risk. Your body regulates levels of estrogen throughout your life to trigger menstrual cycles and menopause. When you become pregnant, your body also begins making more progesterone. These hormones play a role in your overall vein health.
High levels of these hormones during pregnancy may dilate and weaken your veins, which can lead to varicose veins. Progesterone is also known to damage blood vessel valves, causing blood to flow backward and pool in your superficial veins.
Your blood volume significantly increases during pregnancy to accommodate your growing baby. All of this extra fluid puts added pressure on your veins, especially in your thighs and lower legs. The weight of your uterus pushes on the veins in your pelvis, putting even more pressure on them. Altogether, these factors increase your risk of varicose veins.
For the most part, these veins are temporary and often go away once your baby is born. However, if you become pregnant again, they may become worse.
Older Age and Menopause
As we age, our veins lose their elasticity, making it harder for them to widen and constrict to accommodate blood flow. The damaged veins cannot move blood as well as they used to, causing it to pool in your legs. Our skin becomes thinner and also loses its elasticity, making varicose veins just under the surface much more visible.
Women going through menopause (typically between the ages of 40 to 50) are at a higher risk of developing varicose veins. Menopause causes hormone levels to drop, which can weaken and damage blood vessels. You may also experience weight gain, which further increases the risk of varicose veins.
Sitting or Standing for Long Periods of Time
If you stand or sit for long periods of time throughout your day, you are more likely to develop varicose veins. You need to walk or move your legs in order for your calf muscles to squeeze blood from your veins back toward your heart. Without this pumping action, blood begins to pool in your feet and legs, which increases pressure and damages your veins.
Teachers, cashiers, and other professionals who stand in the same place for most of the day often have varicose veins. On the other hand, office workers who sit at a desk all day and people who lead more sedentary lifestyles are also at an increased risk.
Smoking and Other Lifestyle Choices
While you cannot control your genetics, you can control the lifestyle choices you make that impact your vein health. Smoking causes inflammation and blood vessel constriction, limiting the amount of blood that can flow through them. This increases blood pressure, and over time can damage your blood vessels and valves. Not only can smoking cause varicose veins, but it can also contribute to CVI and other venous diseases.
Being overweight or obese also increases the risk of varicose veins. Extra body weight puts added pressure on the blood vessels in your legs, which can damage them over time. People who are overweight or obese may also have high blood pressure, diabetes, or other health complications that contribute to their risk of varicose veins.
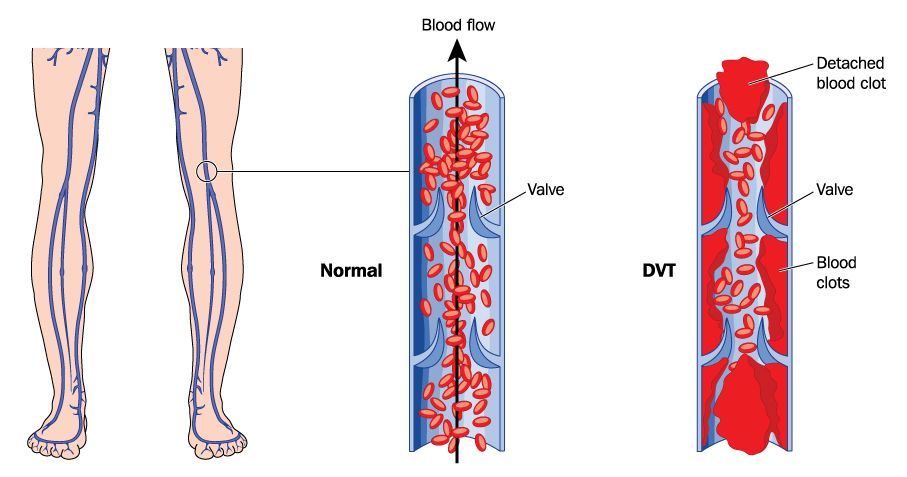
Deep Vein Thrombosis
Deep vein thrombosis (DVT) is a condition that occurs when a blood clot forms in a “deep” vein in your leg, pelvis, or abdomen. The blood clot blocks blood flow through your vein, causing pressure to build behind it. Over time, this pressure damages the valves, causing varicose veins.
If left untreated, DVT can lead to other vein complications. It also increases your risk of pulmonary embolism (PE), which occurs when a blood clot breaks off and travels from your legs to your lungs. The clot becomes stuck, blocking blood flow and increasing pressure within your lungs. As a result, you may experience chest pain and shortness of breath.
To learn more about DVT and venous thrombosis,
read here.
Symptoms of Varicose Veins
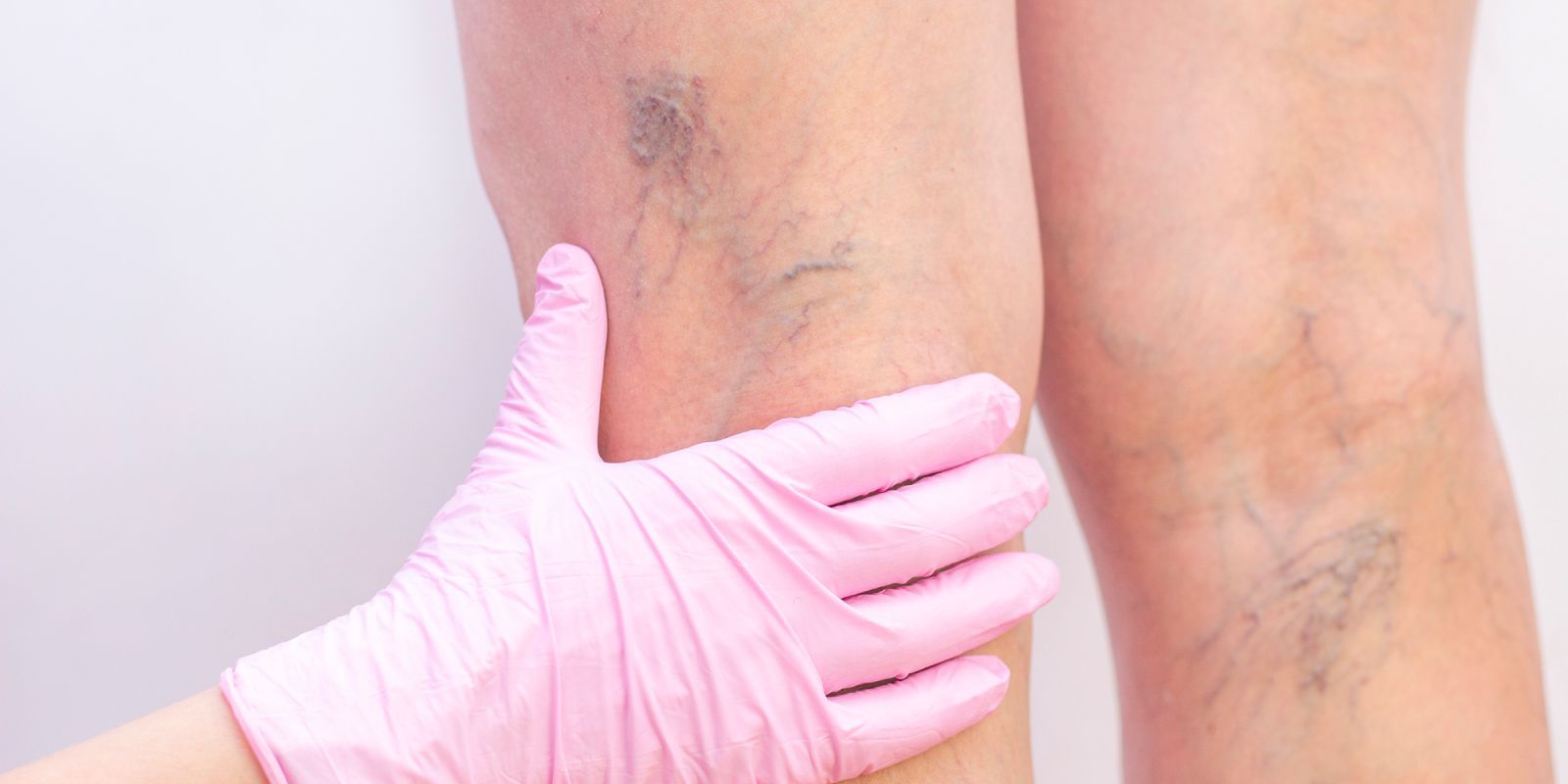
When you think of varicose veins, you likely think of blue, twisted, or bulging veins just beneath the surface of the skin. However, you may also experience other symptoms related to underlying vein issues, such as:
- Swelling in your legs or ankles
- A feeling of fullness, heaviness, or aching pain in your legs or feet, especially after exercising
- Itching sensation around the veins
- Leg cramps at night (known as nocturnal leg cramps)
- Skin discoloration around the veins
- Open sores or ulcers on your legs
In more severe cases, varicose veins can interfere with your daily activities and mobility. They may get worse throughout the day or when you spend long periods of time on your feet. However, these symptoms usually go away when you rest and elevate your feet and legs.
Varicose Veins Versus Spider Veins
If you have varicose veins, you may have also noticed smaller, red-colored veins that look like spider webs just underneath your skin. These are known as
spider veins (or telangiectasias), and they form when the smaller blood vessels in your legs become damaged. Unlike varicose veins, spider veins do not cause your skin to bulge out. They are typically caused by hormonal changes, a leg injury, or exposure to too much sunlight. Generally, spider veins are harmless, but they may be a sign of blood vessel damage in your legs.
How are Varicose Veins Diagnosed?
In most cases, varicose veins can be diagnosed with a simple physical exam. Your doctor or vein specialist will inspect your legs to look for varicose veins, spider veins, and other signs of venous insufficiency. They will also if you have been experiencing any other symptoms and what helps you to manage them.
They may also order an ultrasound to take detailed images of your veins. A Doppler ultrasound uses sound waves that bounce off your blood cells and blood vessels. These sound waves create images that help your doctor or vein specialist look for damaged valves or blockages from blood clots.
Varicose Vein Treatments
If you are looking to get rid of varicose veins and enhance the look of your legs, your doctor may refer you to a vein specialist or vascular surgeon. These professionals are specially trained in treating vein issues to improve your skin’s appearance and alleviate uncomfortable symptoms.
While there is no cure for varicose veins, they can be managed with compression therapy and minimally invasive treatments. Your
vein specialist will go over the different treatment options and choose which is best for you.
Compression Therapy and Elevation
Your doctor or vein specialist will likely recommend compression therapy and elevation to combat swelling and encourage blood flow back toward your heart. Compression therapy involves using specially made garments that apply pressure to your feet, ankles, and legs. This pressure helps move blood back into your deep veins and out of your legs. There are a few different types of compression garments used to manage varicose veins and venous insufficiency.
Compression Stockings
Compression stockings are the most common type of compression therapy. These long socks squeeze the most at your ankles and gradually lessen as they move up your leg. Your doctor or vein specialist will prescribe a certain level of pressure based on how severe your symptoms are. You will wear compression stockings for several hours throughout the day, especially if you stand or sit for most of it.
Compression Bandages
Compression bandages are the preferred compression therapy for people with ulcers caused by varicose veins. These long pieces of elastic wrap are wrapped around your ankles and legs by a healthcare professional. Dressings can be applied under the bandages to help heal ulcers and keep your skin dry. It is important to get your compression bandages changed at least once a week to keep them clean and dry.
Using Compression Therapy
You may notice some discomfort when starting compression therapy — this is normal and it should continue to improve as you use your stockings or bandages. Your doctor or vein specialist will also recommend elevating your feet and legs above your heart. Gravity helps move pooled blood in your legs back toward your heart to reduce swelling. Try sitting or lying down when possible throughout the day, and prop your feet and legs up with pillows or blankets.
If your compression garments are still uncomfortable and are making it difficult to stick to your treatment plan, talk to your doctor or vein specialist. They can offer you tips and advice, or they may recommend a new compression therapy to try.
Be sure to let your doctor know if you have peripheral artery disease (PAD). This condition is caused by the buildup of fatty deposits (known as plaques) in your blood vessels. Compression therapy may be harmful if you have PAD, so they will recommend a different treatment plan for you.
Minimally Invasive Treatments
Your vein specialist may also recommend a minimally invasive treatment to help clear away varicose veins or remove them entirely. These treatments use local anesthesia and a long, thin, flexible tube known as a catheter which is inserted through a small incision in your leg. There are very few side effects with minimally invasive techniques, helping you heal and recover quickly.
Sclerotherapy
Sclerotherapy is used to treat small varicose veins and associated spider veins. During this procedure, the doctor will insert a thin needle into the affected vein and inject a liquid or foam chemical solution. This causes the vein to collapse in on itself, preventing it from carrying any blood. Between 50 to 80 percent of people see results within a few months after treatment. To learn more about sclerotherapy, read here.
Phlebectomy and Ablation
A phlebectomy is used to completely remove varicose veins near the surface of your skin. The doctor will create small incisions over the damaged vein and use a phlebectomy hook to remove it.
This procedure is typically combined with radiofrequency ablation, which uses a catheter with a specialized tip that creates radio waves. These waves generate heat that seals the vein from the inside so it can no longer carry blood to your deep veins. Nearly all patients see success with this treatment for many years. Read here to learn more about
phlebectomy and
radiofrequency ablation.
ClariVein
ClariVein is another minimally invasive procedure that uses a specialized catheter with a rotating tip. This tip mechanically destroys the varicose vein while also delivering a chemical (similar to sclerotherapy) to help seal it off. The catheter used in ClariVein is much smaller than the one used in other procedures and requires a smaller incision. To learn more about ClariVein, read here.
VenaSeal
VenaSeal uses a medical-grade adhesive to close off varicose veins, preventing them from carrying blood. This redirects blood to your healthy veins, helping it flow away from your legs and back toward your heart. Since VenaSeal does not use heat or destroy the vein in any way, there is little to no discomfort. To learn more about VenaSeal, read here.
Surgical Treatments
For more severe varicose veins that cannot be treated with minimally invasive techniques, your vein specialist may recommend vein stripping and ligation. This procedure is more intensive and generally requires sedation to make you sleepy and/or more anesthesia.
The
vein specialist will use ultrasound to find the varicose veins and create large incisions near them. They will tie the vein off (known as ligation) and then remove it entirely from your body (known as stripping). In some cases, your doctor may use ablation instead to close the vein off. In total, the procedure can take between one to three hours.

Preventing and Managing Varicose Veins
If you have varicose veins, there are steps you can take to prevent them from becoming worse or returning after treatment. These lifestyle changes help encourage blood flow back to your heart and take extra pressure off your veins.
Health professionals from New York University recommend eating a healthy diet low in salt to stop your body from hanging onto extra water. This helps lower your blood pressure, preventing varicose veins. The combination of a healthy diet and getting regular movement or exercise can also help you reach a healthy weight, taking extra pressure off your veins.

DR. AMIT POONIA M.D.
Your New Jersey Vein Specialist
Dr. Poonia is double board-certified in interventional pain management and anesthesiology.
Dr. Poonia’s philosophy is based on teamwork, cooperation, and collaboration among his patients’ treatment teams. He believes that healthcare providers work
best when they work together to accurately diagnose a patient’s problem, find effective treatments, and provide maximum rehabilitation and quality of life improvements.
Dr. Poonia customizes his treatment plans based on each patient’s unique characteristics. He employs the latest minimally-invasive technologies to enhance comfort during treatment and to speed recovery.
References
- Anwar MA, Georgiadis KA, Shalhoub J, et al. A review of familial, genetic, and congenital aspects of primary varicose vein disease. Circ Cardiovasc Genet. 2012;5(4):460-466. doi:10.1161/CIRCGENETICS.112.963439.
- Chronic Venous Insufficiency. Cleveland Clinic. July 17, 2022. Accessed January 24, 2023. https://my.clevelandclinic.org/health/diseases/16872-chronic-venous-insufficiency-cvi.
- Ciardullo AV, Panico S, Bellati C, et al. High endogenous estradiol is associated with increased venous distensibility and clinical evidence of varicose veins in menopausal women. J Vasc Surg. 2000;32(3):544-549. doi:10.1067/mva.2000.107768.
- Leg Veins: Why They Appear and How Dermatologists Treat Them. American Academy of Dermatology Association. Accessed January 24, 2023. https://www.aad.org/public/cosmetic/younger-looking/how-dermatologists-treat-leg-veins
- Lifestyle Changes for Varicose Veins. NYU Langone Health. Accessed January 25, 2023. https://nyulangone.org/conditions/varicose-veins/treatments/lifestyle-changes-for-varicose-veins
- Raetz J, Wilson W, Collins K. Varicose veins: Diagnosis and treatment. Am Fam Physician. 2019;99(11):682-688.
- Sclerotherapy. Cleveland Clinic. June 12, 2022. Accessed January 25, 2023. https://my.clevelandclinic.org/health/treatments/6763-sclerotherapy
- Scovell S. Patient Education: Lower Extremity Chronic Venous Disease (Beyond the Basics). UpToDate. September 20, 2021. Accessed January 24, 2023. https://www.uptodate.com/contents/lower-extremity-chronic-venous-disease-beyond-the-basics.
- Tang TY, Kam JW, Gaunt ME. ClariVein® — Early results from a large single-centre series of mechanochemical endovenous ablation for varicose veins. Phlebology. 2017;32(1):6-12. doi:10.1177/0268355516630154.
- van Rij AM, De Alwis CS, Jiang P, et al. Obesity and impaired venous function. Eur J Vasc Endovasc Surg. 2008;35(6):739-744. doi:10.1016/j.ejvs.2008.01.006.
- Varicose Veins. Cleveland Clinic. December 29, 2021. Accessed January 24, 2023. https://my.clevelandclinic.org/health/diseases/4722-varicose-veins
- Varicose Veins. National Heart, Lung, and Blood Institute. March 24, 2022. Accessed January 24, 2023. https://www.nhlbi.nih.gov/health/varicose-veins
- Varicose Veins and Spider Veins. Office on Women’s Health. February 15, 2021. Accessed January 24, 2023. https://www.womenshealth.gov/a-z-topics/varicose-veins-and-spider-veins
- Varicose Veins Stripping and Ligation. Cleveland Clinic. October 19, 2022. Accessed January 25, 2023. https://my.clevelandclinic.org/health/treatments/17614-venous-disease-vein-ligation--stripping
- Varicose Veins While Pregnant. Cleveland Clinic. May 25, 2022. Accessed January 25, 2023. https://my.clevelandclinic.org/health/diseases/23331-varicose-veins-in-pregnancy
- Varicose Veins: Why We Get Them and What Can Help. University of Rochester Medical Center. April 6, 2017. Accessed January 24, 2023.